12.4: Sexually Transmitted Infections (STIs aka STDs)
- Page ID
- 167229
Sexually transmitted infections (STIs) are passed via sexual activity from person to person. They can be passed with vaginal, anal or oral sex and in the case of oral herpes, via kissing. These infections can be caused by bacteria, viruses or parasites. Some are passed with bodily fluids and others by skin-to-skin contact. STIs are also referred to as sexually transmitted diseases or STDs.
According to the most recent compiled CDC data from 2018, almost half of all new STI’s are in young people ages 15-24, so it is important to keep in mind that this age group is at higher risk (CDC, 2018).
Often, there are no symptoms, so the only way to know for sure if an STI is present is to do a test. Routine testing can be a good idea for all people who are sexually active. How often to test and what to test for depends on several factors. It is recommended to speak with a medical professional if you have questions about testing.

General Testing Guidelines
- At a minimum, everyone should do at least one lifetime HIV test
- Everyone who is sexually active test at least once a year for HIV
- For MSM (men having sex with men or guys having sex with guys) testing is recommended every 3-6 months
- For people with multiple partners every 3-6 months
- People who are on PrEP (pre exposure prophylaxis) for HIV prevention testing every three months
- About three weeks post incident of concern, such as unprotected sex
- If having symptoms (such as burning with urination or genital discharge) test AND see a medical provider.
- If a partner or previous partner shares they have an STI. In this case, also seek treatment from a medical provider.
A Long History of Stigma
There has been stigma around STIs since there have been STIs. One good example is the case of syphilis.
Excerpt from Brief History of Syphilis:
From the very beginning, syphilis has been a stigmatized, disgraceful disease; each country whose population was affected by the infection blamed the neighboring (and sometimes enemy) countries for the outbreak. So, the inhabitants of today’s Italy, Germany and United Kingdom named syphilis ‘the French disease,’ the French named it ‘the Neapolitan disease,’ the Russians assigned the name of ‘Polish disease,’ the Polish called it ‘the German disease,’ The Danish, the Portuguese and the inhabitants of Northern Africa named it ‘the Spanish/Castilian disease’ and the Turks coined the term ‘Christian disease.’ Moreover, in Northern India, the Muslims blamed the Hindu for the outbreak of the affliction. However, the Hindu blamed the Muslims and in the end, everyone blamed the Europeans (Tampa et al, 2014).
In the 16th and 17th centuries, syphilis was thought to be punishment for sin, and some felt people with the disease didn’t deserve treatment.
Although there has been much medical advancement in the treatment of STIs, the stigma has not completely gone away. Many people report feeling dirty or ashamed if they have an STI, primarily because this is what culture tells us. Rather than seeing it the way we see other contagious infections, such as colds, there is the added layer of shame because we still see sex as shameful in some contexts in our culture.
With HIV and AIDS, there was added stigma due to homophobia that already existed, because it was largely affecting the gay male community. HIV gave people a new reason to express hatred and fear of gay men, as they were now seen as vectors of disease.
One way to combat stigma around STIs is to normalize that when we touch bodies, when we are sexual, we may pass bacteria and viruses around. It’s part of being sexual beings. Anyone can get an STI. It doesn’t say anything about their moral character or who they are as a person.
Bacterial Infections
The most common bacterial STIs are chlamydia, gonorrhea and syphilis. Less common ones are chancroid and mycoplasma genitalium. Bacterial infections are curable with antibiotics.
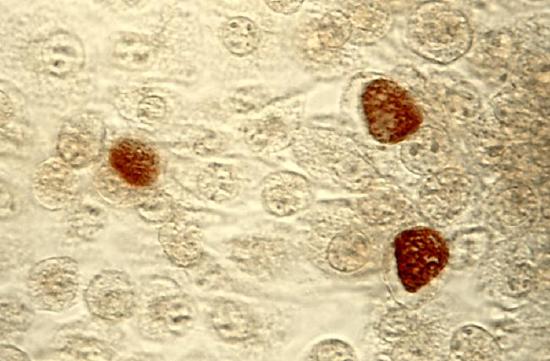
Chlamydia
Chlamydia is caused by chlamydia trachomatis and is the most common bacterial STI in the United States, with highest rates among females under age 24. If left untreated for an extended period, it may result in urethritis, epididymitis, cervicitis, or acute salpingitis (inflammation of the fallopian tubes).
Symptoms for people with vulvas may include vaginal discharge, post-coital and intermenstrual bleeding, dysuria (painful or difficult urination), lower abdominal pain, and deep dyspareunia (vaginal pain before, during or after intercourse).
Symptoms for people with penises may include urethral discharge, dysuria, urethritis, and possible epididymitis.
Testing specimens may be obtained via a urine sample from patients of all genders. It is also possible to do endocervical or vulvovaginal swabs on vulvas and urethral swabs on penises. Rectal swabs are recommended for those who receive anal sex, and oropharyngeal (throat) swabs for those who have given oral sex. Self-swabbing may be available for throat, rectal and possibly for vaginal swabs.
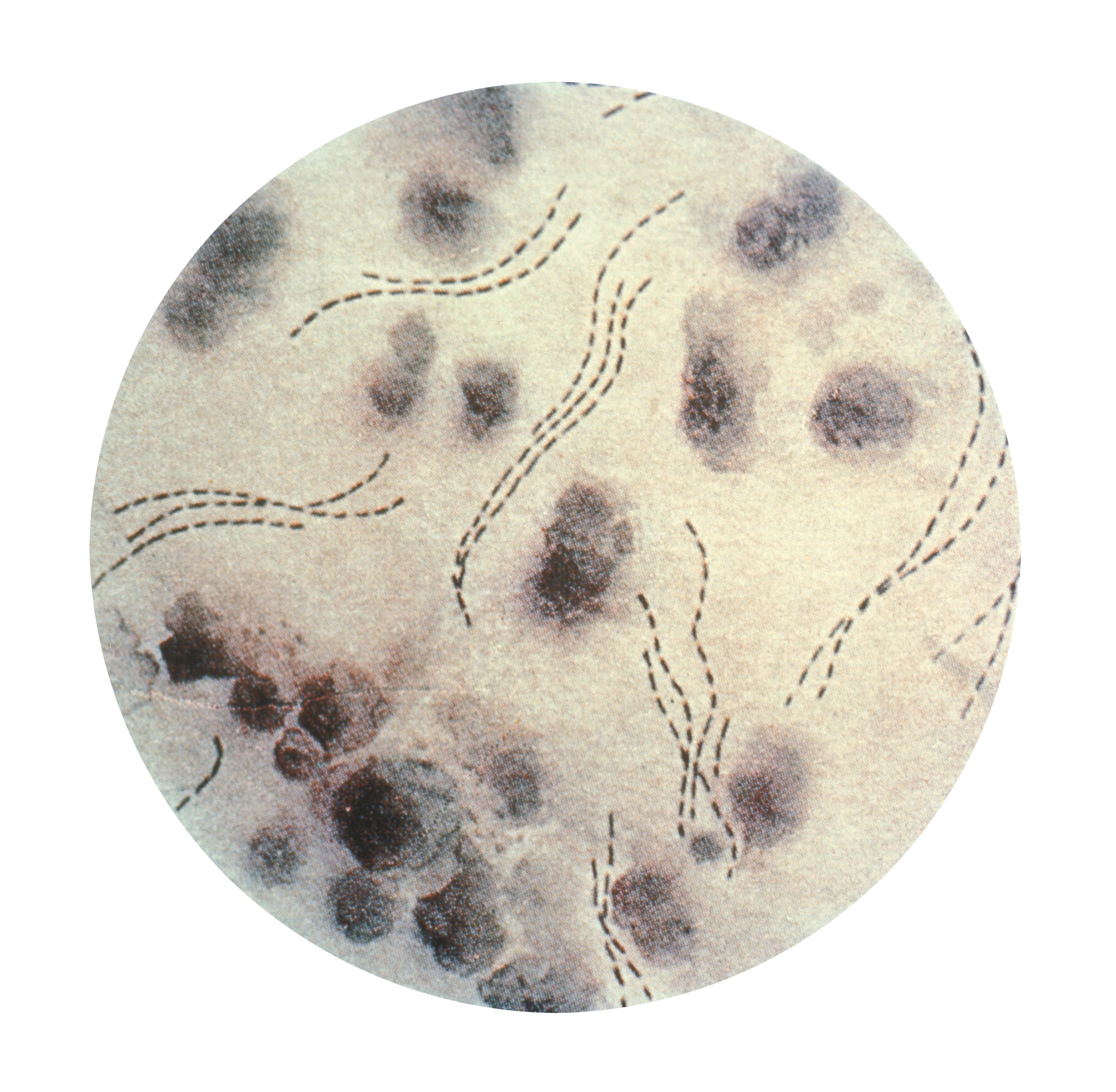
Gonorrhea
Gonorrhea is due to infection by the bacterium Neisseria gonorrhoeae. The most common symptoms are vaginal or penile discharge and dysuria. Other symptoms may include abdominal pain during intercourse, bleeding between menstrual periods, and post coitus or pain or swelling of testes.
It can affect the cervix, uterus, and fallopian tubes, and the urethra, mouth, throat, eyes, and anus and lead to inflammation including urethritis, cervicitis, proctitis, salpingitis, or pharyngitis.
Untreated infection is a cause of PID (pelvic inflammatory disease) and can result in tubal scarring that may lead to infertility or ectopic pregnancy. Mothers who acquire gonorrhea during pregnancy can pass the infection to the fetus, possibly causing blindness or life-threatening infections. The testing options are the same as chlamydia.

Syphilis
Syphilis is caused by infection with Treponema pallidum, a spirochete bacterium. It has several potential stages- primary, secondary, latent and tertiary (late) and neurosyphilis. Transmission occurs through direct contact with an infectious chancre (lesion) via vaginal, anal or oral sex.
Congenital syphilis is passed during pregnancy or labor, and can result in abnormalities in the fetus. Syphilis infection in pregnant women increases the risk of miscarriage and stillbirth.
Treponema pallidum infection is diagnosed with an antibody blood test. If that test shows reactive (which means positive), then further testing is done. Rapid plasma reagin (RPR) testing is done to confirm positive treponemal testing.

Chancroid
Chancroid is not a common STI in the United States. In order to make a diagnosis of chancroid, four criteria must be met. 1) one or more painful genital ulcers; 2) swollen lymph nodes; 3) syphilis has been ruled out as a cause of the ulcers; 4) herpes has also been ruled out as a cause of the ulcers. Symptoms usually improve within 3-7 days post treatment.
Mycoplasma Genitalium
M. genitalium causes symptomatic and asymptomatic urethritis (inflammation of the urethra) among men and is the cause of approximately 15%–20% of NGU (non gonococcal urethritis or urethritis that is not cause by gonorrhea), 20%–25% of nonchlamydial NGU, and 40% of persistent or recurrent urethritis.
M. genitalium is associated with cervicitis, PID (pelvic inflammatory disease), preterm delivery, spontaneous abortion, and infertility. M. genitalium infections among women are frequently asymptomatic, yet the consequences associated with asymptomatic infection are unknown.
Testing is not recommended if there are no symptoms. Only if there is recurrent urethritis, cervicitis or PID, then testing is recommended. There has been resistance to some antibiotics for treatment.

"Schematic illustration of interior of ''Mycoplasma genitalium'' with increasing levels of detail in parts B and C" by Isseki Yu et al is licensed under CC BY 4.0
Parasitic Infections
Parasitic STIs include trichomoniasis, pubic lice, and scabies. They are all curable with antibiotics and other medications.
Trichomoniasis (or “trich”) is very common but not routinely tested for. It is caused by infection with a protozoan parasite called Trichomonas vaginalis. Most people do not have any symptoms. If there are symptoms, they range from mild to severe, can come and go, and may include itching or irritation inside the penis, itching, redness or soreness of genitals, burning after urination or ejaculation, penile discharge, and increased vaginal discharge that can be clear, white, yellowish or greenish with a fishy odor. A test can be done with a sample of vaginal fluid or urine.
Pubic Lice are also called crabs or crab lice as they have a crab-like appearance. They are different from head and body lice. They are passed during sexual activity and diagnosed by finding a louse or eggs in the pubic area. Over the counter treatment lotion is available.
Scabies is a contagious skin condition caused by the human itch mite (Sarcoptes scabiei var. hominis). It is spread via direct and prolonged skin-to-skin contact and therefore can be spread during sexual activity, but can also be spread through casual contact or transmitted via clothing or bedding. Symptoms include intense itching and a pimple-like skin rash. Treatment is a prescription medicine known as scabicide, as it kills scabies mites.
Viral Infections
Viral STIs include HSV (herpes simplex virus), HPV (human papilloma virus) and HIV (human immunodeficiency virus), which can lead to AIDS (acquired immune deficiency syndrome). They are not curable, but they are treatable.
Herpes
Herpes is caused by HSV (herpes simplex virus) 1 or 2. Traditionally we have associated HSV 1 with oral herpes (cold sores on the lips) and HSV 2 with genital herpes. Either strain can be passed with oral sex, so it is possible to find HSV 1 in the genitals and vice versa. Herpes is spread with skin-to-skin contact. It is far more likely to be passed with an active outbreak, but it is not impossible to pass otherwise. There can be viral shedding, when the virus is shedding at the surface of the skin, but the person is not aware. It can be passed with kissing, vaginal, anal or oral sex. It is manageable, but not curable. There is a lot of stigma around having herpes, but it is helpful to know that it is possible to have a happy, healthy sex life with herpes or with a partner who has herpes. In some ways, the stigma is actually worse than the infection itself. The best way to test for herpes is when there is an active outbreak. A medical professional can take a sample of a potential herpes sore to test for the virus itself. There is an antibody blood test available, but it is often not recommended as it is not considered reliable or helpful in most cases. For more on this, STIs aren't a consequence. They're inevitable. | Ella Dawson | TEDxConnecticutCollege

Human Papilloma Virus (HPV)
Gregory Barnell, Nurse Practitioner is credited for the following section.
Human papillomavirus (HPV) is a family of more than 140 viral strains, roughly 40 of which infect the mucosal skin of our bodies — mouth/throat, genitals and anus — and are sexually transmitted by skin-to-skin contact. Other HPV strains infect other types of skin, for example hands, feet or elbows. HPV is never a systemic infection; it can only live in the squamous cells of human skin.
Sexual transmission of HPV is very common. Almost all unvaccinated people who have sex with other people will acquire HPV. Most HPV infections clear on their own, without any obvious disease (change to the skin). There is no treatment for HPV itself, which means that screening for HPV is not clinically useful or recommended as a public health measure, except as part of cervical cancer screening programs. About 20% of people with HPV express disease. In these people, low-risk HPV strains cause warts (in mouth, anus or genitals) and high-risk strains cause pre-cancerous lesions in the same areas. Both warts and precancerous lesions can also clear (go away) on their own, without treatment; however, since anogenital warts are a risk factor for HIV infection, it is generally recommended to treat warts.
Long-term infection with high-risk HPV, particularly HPV-16 and -18, poses a higher risk for cancer. Cervical cancer can develop more quickly and is much more frequent than other sites where HPV infection occurs. Cervical cancer screening (Pap screening and high-risk HPV testing) is very successful at preventing most cervical cancer. All people with a cervix should be periodically screened for cervical cancer, starting at age 25 and ending at age 65. Cancers of the anus, penis, vulva, vagina and mouth/throat are very rare in the general population. When they do occur, this is much more likely later in life. No specific recommendation exists to screen for these other HPV-associated cancers, although many experts recommend anal cancer screening for people with HIV (PWH), especially for older PWH who are men who have sex with men (MSM). Mouth and throat cancer is screened for during dental visits.
Available vaccines are very effective at preventing HPV infections and diseases caused by HPV. Most pediatricians recommend HPV vaccination at age 11-13, although the vaccine is FDA (Federal Drug Administration) approved up to age 45. The CDC recommends “catch up” vaccination up to age 26, for all people who were not vaccinated as a pre-teen.
-Gregory Barnell, NP
Human Immunodeficiency Virus (HIV)
Human Immunodeficiency Virus (HIV) is the virus that may cause AIDS. AIDS is acquired immunodeficiency syndrome. Not everyone with HIV gets AIDS. HIV attacks the immune system, and if it is not treated, can lead to illness and death. There is no cure for HIV, but there is treatment. Today people who are HIV positive (have the HIV virus) can live long healthy lives if they are receiving good medical care. This often means taking HIV medicines and having one’s viral load (the amount of HIV in the blood) tested routinely.
The only way to know for sure if someone has HIV is to get tested. Testing can be done with a blood sample in a laboratory or at some testing sites, rapid preliminary testing can be done with a mouth swab or a finger prick. This testing is considered preliminary because it is not as accurate as giving a blood sample. If a rapid oral or finger prick test is positive, a follow up blood test is recommended to confirm a diagnosis of HIV.
Getting to Zero
Getting to zero is a campaign that was started by UNAIDS in 2010 and has been adopted around the world as a vision for ending the HIV/AIDS epidemic. It refers to zero new HIV infections, zero deaths from AIDS and zero stigma around HIV/AIDS. We now have several tools to help with this vision.
There is a medication that can be taken daily to prevent HIV known as PrEP which stands for pre-exposure prophylaxis. People can also take it as needed which is referred to as on-demand PrEP or PrEP 2:1:1. That works for people whose sexual activity is not that frequent and always planned ahead because in order for the medicine to work the first two pills must be taken 2-24 hours prior to sexual activity. For people who don’t fit this profile, taking daily PrEP makes more sense. People who are on PrEP are usually required to do lab tests every 3 months including HIV and full STI testing.
PEP stands for post-exposure prophylaxis and refers to medicine taken after a possible HIV exposure. This medicine must be taken within 72 hours after the potential exposure in order for it to work.
U=U means undetectable equals untransmittable and refers to people who are HIV positive who cannot transmit the virus. If someone is positive but their viral load (the amount of HIV in their system) is well controlled and low, also known as undetectable, they cannot give someone else HIV. These are all powerful tools in the fight to end the HIV/AIDS epidemic.
A history of AIDS Activism in the United States
ACT UP (AIDS Coalition to Unleash Power) was a non-violent activist group started in New York City in 1987. It was a response to the U.S. government’s severe mishandling of the HIV/AIDS crisis. ACT UP used direct action to pressure government agencies and pharmaceutical companies to pay attention to the AIDS crisis. It was mostly affecting MSM and IV drug users, and was being largely ignored.
In 1988, ACT UP staged a sit-in of over 1000 activists and successfully shut down the FDA (Food and Drug Administration) headquarters for a day, protesting the slow process of drug approval for HIV medications. It was one of their most successful protests as it resulted in the FDA agreeing to speed up the process.
The Names Project AIDS Memorial Quilt is another example of early AIDS activism. Cleve Jones, an activist in San Francisco, had people make signs with the names of loved ones they had lost to AIDS complications and the signs were hung on the old San Francisco Federal Building, as part of a candlelight march in 1985. Jones reports that when he saw the signs posted there, they looked like a patchwork quilt to him and he was inspired with the idea of creating an actual quilt to memorialize the lives lost to the AIDS crisis. The quilt became both a place for lovers, families and friends to honor their loved ones, but also a powerful political statement as it continued to grow in size and panels from all over the country were added.
“Today, the AIDS Memorial Quilt is an epic 54-ton tapestry that includes nearly 50,000 panels dedicated to more than 105,000 individuals. It is the premiere symbol of the AIDS pandemic, a living memorial to a generation lost to AIDS and an important HIV prevention education tool. With hundreds of thousands of people contributing their talents to making the memorial panels, and tens of thousands of volunteers to help display it, the Quilt is considered the largest community arts project in history” (The History of the Quilt, n.d.)



