We will provide several examples of health disparities next, followed by a discussion of what factors contribute to those disparities. Health disparities refer to preventable differences in health outcomes or access to healthcare across different social groups. The National Institute on Minority Health and Health Disparities (2025) defines health disparities as:
"largely preventable health differences that adversely affect populations who experience greater challenges to optimal health and are closely linked with intergenerational social, economic, and/or environmental factors," which "may be observed in the risks, prevalence, or problems resulting from specific behaviors, as well as the incidence, prevalence, and mortality from conditions, diseases, and/or disorders. Health disparities also can be observed in health care access, quality, and utilization, and within the delivery of clinical care."
Health disparities can be found across all social groups, such as regarding social class, race, gender/sex, sexuality, and age. We will explore some of these disparities now.
Social Class
There has been growing recognition in the government and in medical and academic communities that social class influences health outcomes (Centers for Disease Control and Prevention 2011; Patel 2020).
Marilyn Winkleby and her research associates (1992) state that "one of the strongest and most consistent predictors of a person’s morbidity [incidence of disease] and mortality [death] experience is that person’s socioeconomic status (SES). This finding persists across all diseases with few exceptions, continues throughout the entire lifespan, and extends across numerous risk factors for disease." In other words, being in a lower social class makes you more likely to get sick or die of disease than people in a higher social class.
Many types of health indicators illustrate the social class–health link in the US. In an annual survey conducted by the government, people are asked to indicate the quality of their health. In 2024, nearly 15% of the adult population reported being in poor or fair health, but over 29% of those at <100% of the federal poverty level (FPL) reported being in poor or fair health, compared with less than 11% of those at 200% of the FPL or higher (NCHS 2025). Poor people are much more likely than those with higher incomes to say their health is only fair or poor. These self-reports of health are subjective indicators, and it is possible that not everyone interprets 'fair' or 'poor' health in the same way. But objective indicators of actual health also indicate a strong social class–health link (NCHS 2011).

This chart shows how rates of poor or fair perceived health are far higher among adults at less than 100% of the federal poverty level (FPL) than those who have higher socioeconomic standing (at 200% or higher of the FPL).
Source: NCHS 2025
Poor adults are also at much greater risk for many health problems, including heart disease, diabetes, arthritis, and some types of cancer. Rates of high blood pressure, serious heart conditions, and diabetes are at least twice as high for middle-aged adults with family incomes below the poverty level than for those with incomes at least twice the poverty level. All these social class differences in health contribute to a striking difference in life expectancy, with Americans whose family incomes are more than four times the federal poverty level expected to live 6.5 years longer than those living in poverty (Kaplan 2009).
Several reasons account for the social class–health link (Pampel, Krueger, & Denney 2010). One reason is stress. Because people with a lower socioeconomic status experience financial insecurity, they can be more stressed. For instance, stress is higher for people with low incomes because of unemployment, problems in paying for the necessities of life, and a sense of little control over what happens to them. Stress in turn damages health because it weakens immune systems, making it difficult to fight viruses and to heal.
Second, social class also influences how likely you are to have health insurance and get good health care. As is well known, many poor people lack medical insurance and in other respects have inadequate health care. These problems make it more likely they will become ill in the first place and more difficult for them to become well because they cannot afford to visit a physician or to receive other health care. Still, social class disparities in health exist even in countries that provide free national health care, a fact that underscores the importance of the other reasons discussed here for the social class–health link (Elo 2009). Particularly in the US, where healthcare is not universal, the poorer you are, the less likely you are to have quality health insurance.
Suppose you have a full-time, beneficial managerial job in a large multinational corporation. In that case, you will likely receive paid time off, excellent health insurance, long-term care insurance, and contributions to your retirement. This package of benefits helps you to prevent disease and stay healthy. Conversely, suppose you have a low-wage seasonal job, particularly in a state that doesn’t fully participate in the Affordable Care Act (ACA). In that case, neither your employer nor the government provides health care insurance for you. You pay for your healthcare out of your own pocket. Given the high cost of care, you will likely delay getting treatment, not have access to preventative care, or not be able to pay for complex treatment. In the US, economics, insurance, and health outcomes are linked in enormously inequitable ways.
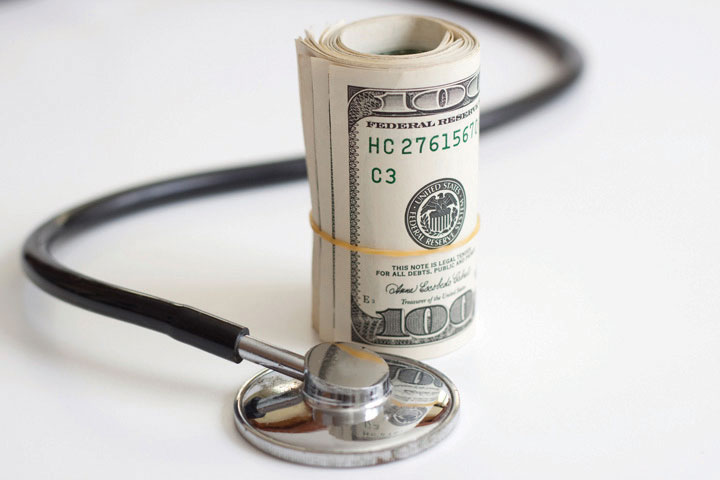
Many people who are poor or near poor lack medical insurance and in other ways have inadequate health care. These problems make it more likely they will become ill and, once ill, less likely they will become well.
© Thinkstock
Third, education influences health outcomes. Ae lack of education leads poor people to be unaware or unconcerned about risk factors for health and to have a fatalistic attitude that promotes unhealthy behaviors and reluctance to heed medical advice (Elo 2009). General level of education matters here. In one study of whether smokers quit smoking after a heart attack, only 10% of heart attack patients without a high school degree quit smoking, compared to almost 90% of those with a college degree (Wray, Herzog, Willis, & Wallace 1998). Education about medicine and health is important as well. For instance, Phelan and Link (2003) note that many behavior-influenced diseases like lung cancer, coronary artery disease, and HIV/AIDS initially were widespread across social class groups. However, once information linking habits to disease was shared, these diseases decreased in higher social class groups and increased in lower social class groups. This illustrates the important role of education initiatives regarding a given disease and possible inequalities in how those initiatives effectively reach different groups.
A fourth reason for social class health disparities is that poor people live in conditions, including crowded, dilapidated housing with poor sanitation, that are bad for their health and especially that of their children. Although these conditions have improved markedly in the US over the last several decades, they continue for many of the poor. Crowding was one cause of the higher rates of COVID-19 illness and death among lower-income people.
A final reason for the poor health of poor people is unhealthy lifestyles. Poor people are more likely to smoke, to eat high-fat food, to avoid exercise, and to be overweight (Pampel et al. 2010). However, we must keep in mind that health habits are constrained by structural factors such as living in food deserts, lacking access to quality healthcare, and having less education on health habits.
Covid-19 death tolls in the US demonstrate the relationship between health and poverty. For instance, Finch and Finch (2020) found that residents of poorer counties were more likely to die from Covid-related deaths than those who resided in middle- and high-income counties.
Children and Our Future
The Poor Health of Poor Children
When we consider health disparities, some of the most unsettling evidence involves children. As a recent report by the Robert Wood Johnson Foundation concluded, “The data illustrate a consistent and striking pattern of incremental improvements in health with increasing levels of family income and educational attainment: As family income and levels of education rise, health improves. In almost every state, shortfalls in health are greatest among children in the poorest or least educated households, but even middle-class children are less healthy than children with greater advantages.”
Some government data illustrate the difference that poverty makes for the nation’s children:
- Children of poor mothers are more than twice as likely as children born to wealthier mothers to be born with low birth weight.
- By the age of 9 months, poor children are already more likely to exhibit poor health and lower cognitive and socioemotional development.
- By age 3, poor children are two-thirds more likely to have asthma than children whose families’ incomes are more than 150% of the poverty line.
- Based on their parents’ reports, poor children are almost five times more likely (33% compared to 7%) to be in less than very good health (i.e., their parents rated their children’s health as poor, fair, or good rather than as very good or excellent).
In these and other ways, children in low-income families are more likely than children in wealthier families to have more health problems, many of which last into adolescence and adulthood. Poor children’s poor health thus makes a critical difference throughout their lives. As sociologist Steven A. Haas and colleagues observe, “A growing body of work demonstrates that those who experience poor health early in life go on to complete less schooling, hold less prestigious jobs, and earn less than their healthier childhood peers.”
One reason for the poor health of poor children is that their families are more likely to experience many kinds of stress. Another reason is that their families are more likely to experience food insecurity and, if they are urban, to live in neighborhoods with higher levels of lead and pollution. Low-income children also tend to watch television more often than wealthier children and for this and other reasons to be less physically active; their relative lack of physical activity is yet another reason for their worse health. Finally, their parents are much more likely than wealthier parents to smoke cigarettes; the secondhand smoke they inhale impairs their health.
The clear evidence of poverty’s effects on the health of poor children underscores the need of the US to do everything possible to minimize these effects. Any money spent to reduce these effects will pay for itself many times over throughout these children’s lifetimes: They will have fewer health problems as they grow up, costing the US much less in health care, and be better able to do well in school and to have higher incomes as adults. In both the short run and long run, then, improving the health of poor children will also improve the economic and social health of the whole nation.
Sources: Haas, Glymour, & Berkman 2011; Kaplan 2009; Murphey, Mackintosh, & McCoy-Roth 2011; Robert Wood Johnson Foundation 2008
Sociologists also see unequal outcomes when they examine prevalence and outcomes of mental illness. One of the most consistent findings across studies is that lower social class groups have greater amounts of mental illness. For instance, poor people have higher rates of severe mental illnesses such as schizophrenia, serious depression, and other problems (Mossakowski 2008; Ridley et. al 2020). Why is this the case?
One of the earliest studies of the sociology of mental health came from the University of Chicago in the 1930s. Sociologists explored whether mental illness caused poverty or whether poverty caused mental illness. The two researchers who led this project, Faris and Dunham (1939), looked at psychiatric admissions to Chicago hospitals by neighborhood. What they found was rather shocking: There was a nine times increased rate of schizophrenia from people who came from poorer neighborhoods than from middle-class neighborhoods. The researchers tried to figure out why.
One idea was social selection, the idea that lower class position is a consequence of mental illness. Mentally ill people would drift downward into lower income groups or poorer neighborhoods because they couldn’t keep jobs. In addition to considering social selection, they considered social causation. In this model, which Faris and Dunham later refuted, lower class position was a cause of mental illness.
Results of this early study came back mixed. At first, Faris and Dunham said that the isolation and poverty of living in the central city created schizophrenia – a cause. But then, they changed their minds and said people with schizophrenia have downward drift and moved to the central, poorer part of town after developing schizophrenia – an effect. Later studies have found that Faris and Dunham’s study was actually trying to tell us that it’s both – cause and effect. Social selection theories and social causation theories can be used to account for the relationship between schizophrenia and poverty.
Thus, as with physical health, poverty itself can be a risk factor for poor mental health. Although there is evidence of both causal paths, most scholars believe that poverty contributes to mental illness more than the reverse (Warren 2009). This article from the Guardian, Mental Illness and Poverty: You Can’t Tackle One Without The Other, might help you to make more sense of this complex relationship.
Further, people with mental health issues can struggle with educational and economic stability because sufficient social supports are not in place to support them, resulting in stagnant or downward social mobility.
Race
When looking at the social epidemiology of the US, it is easy to see health disparities between people with different races/ethnicities. These disparities can be a matter of life and death. The discrepancy between Black and white Americans shows the gap clearly. In 2018, the average life expectancy for Black males was 74.7 years. The average life expectancy for white males was 78.5 years. This is a gap of almost 5 years (Wamsley 2021). We see similar disparities when we look at how many babies die or infant mortality (how many people die at a particular time or place). The 2022 infant mortality rates were highest for Black infants and lowest for Asian infants, as displayed in the chart below. Black infants are more than twice as likely as white infants to die before their first birthday. In a related indicator, parental mortality (from complications of pregnancy or childbirth) stands at 8.1 maternal deaths for every 100,000 live births for white childbearers, 7.2 for Latinx childbearers, and a troubling 23.8 for Black childbearers. Maternal mortality for Black women is thus about three times greater than that for the other two groups (Ely & Driscoll 2024).

Infant mortality rate, by maternal race and Hispanic origin: United States, 2021 and 2022. Infant mortality varies significantly by race/ethnicity. What factors do you think contribute to this disparity?
Source: Ely & Driscoll, National Vital Statistics Reports 2024
In other indicators, Black people are more likely than white people to die from heart disease, although the white rate of such deaths is higher than the rates of Asians, Latinos, and Native Americans. Black individuals are also more likely than whites to be overweight and to suffer from asthma, diabetes, high blood pressure, and several types of cancer. Latinos and Native Americans have higher rates than whites of several illnesses and conditions, including diabetes. Black women are three times more likely to dies as a result of pregnancy related complications compared to white women (CDC 2024).
Commenting on all these disparities in health, a former head of the US Department of Health and Human Services said, "We have been—and remain—two nations: one majority, one minority—separated by the quality of our health" (Penn et al. 2000: 102). The examples just discussed certainly indicate that her statement is still true today.
Why do such large racial/ethnic disparities in health exist? To a large degree, they reflect the high poverty rates for Black, Latinx, and Native Americans compared to those for whites. In addition, inadequate medical care is perhaps a special problem for people of color, thanks to unconscious racial bias among healthcare professionals that affects the quality of care that people of color receive.
Several studies use hospital records to investigate whether people of color receive optimal medical care, including coronary bypass surgery, angioplasty, and catheterization. After taking the patients’ medical symptoms and needs into account, these studies find that Black Americans are much less likely than white Americans to receive the procedures just listed. This is true when poor Black people are compared to poor white people and also when the middle-class is compared (Smedley, Stith, & Nelson 2003). In a novel way of studying race and cardiac care, one study performed an experiment in which several hundred doctors viewed videos of Black and white patients, all of whom, unknown to the doctors, were actors. In the videos, each 'patient' complained of identical chest pain and other symptoms. The doctors were then asked to indicate whether they thought the patient needed cardiac catheterization. The Black patients were less likely than the white patients to be recommended for this procedure (Schulman et al. 1999). It is possible, of course, that some doctors are overt racists and decide that the lives of Black people are less worth saving, but it is far more likely that they have unconscious or implicit racial biases that affect their medical judgments. Regardless of the reason, the result is the same: Black Americans are less likely to receive potentially life-saving cardiac procedures simply because they are Black. Institutional discrimination in medicine, then, is literally a matter of life and death.
Scholars are increasingly concluding that the stress of being Black in the US – facing anti-Black racism – is a major factor in health disparities (Geronimus et al. 2010; Williams 2018). An increasing amount of evidence suggests that being Black in a society filled with racial prejudice, discrimination, and inequality takes what has been called a “hidden toll” on the lives of Black Americans (Blitstein 2009). In this way of thinking, Black Americans are much more likely than whites to be poor, to live in high-crime neighborhoods, and to live in crowded conditions, among many other problems. They are also more likely, whether or not they are poor, to experience racial slights, refusals to be interviewed for jobs, and other forms of discrimination in their everyday lives. All these problems mean that Black individuals from their earliest ages grow up with a great deal of stress, far more than what most white individuals experience. This stress in turn has certain neural and physiological effects, including hypertension (high blood pressure), that impair Black Americans’ short-term and long-term health and that ultimately shorten their lives. These effects accumulate over time: Black and white hypertension rates are equal for people in their twenties, but the black rate becomes much higher by the time people reach their forties and fifties. As a news article on evidence of this “hidden toll” summarized, “The long-term stress of living in a white-dominated society ‘weathers’ blacks, making them age faster than their white counterparts” (Blitstein 2009: 48).
An additional reason for racial disparities in health is diet. Many of the foods that have long been part of Black American culture are high in fat. Partly as a result, Black people are more likely than white people to have heart disease and high blood pressure and to die from these conditions (Parra-Medina et al. 2010). In contrast, first-generation Latinx people tend to have diets consisting of beans, grains, and other low-fat foods, preventing health problems stemming from their poverty from being even worse. But as the years go by and they adopt the typical American’s eating habits, their diets tend to worsen, and their health worsens as well (Pérez-Escamilla 2009).
In a significant finding, Black Americans tend to have worse health than white Americans even among those with the same incomes. Several reasons explain this racial gap. One is the extra stress that Black Americans of all incomes face because they live in a society that is still racially prejudiced and discriminatory (Bratter & Gorman 2011), as discussed above. In this regard, studies find that Black and Latinx people who have experienced the most racial discrimination in their daily lives tend to have worse physical health (Lee & Ferraro 2009). Some middle-class Black people may also have grown up in poor families and incurred health problems in childhood that continue to affect them. As a former US surgeon general once explained, “You’re never dealing with a person just today. You’re dealing with everything they’ve been exposed to throughout their lives. Does it ever end? Our hypothesis is that it never ends” (Meckler 1998).

Black Americans have worse health than whites, even when people with the same incomes are compared. One reason for this racial gap is the continuing racial discrimination that Black Americans experience and the stress that accompanies this experience.
© Thinkstock
Another factor contributing to racial differences in health is physical location: Poor people of color are more likely to live in urban areas and in other locations that are unhealthy places because of air and water pollution, hazardous waste, and other environmental problems (Walker 2011). This problem is termed environmental racism (Michney 2011), and will be discussed further in a future chapter. One example of this problem is found in the so-called Cancer Alley on a long stretch of the Mississippi River in Louisiana populated mostly by Black Americans: 80% of these residents live within three miles of a polluting industrial facility (Cernansky 2011).
The evidence on the connection between race and mental health is mixed: Although many studies find higher rates of mental disorder among people of color, some studies find similar rates to whites’ rates (Mossakowski 2008). These mixed results are somewhat surprising because several racial groups are poorer than whites and more likely to experience everyday discrimination, and for these reasons should exhibit more frequent symptoms of mental and emotional problems. Despite the mixed results, a fair conclusion from the most recent research is that Black and Latinx individuals are more likely than white individuals to exhibit signs of mental distress (Jang, Chiriboga, Kim, & Phillips 2008; Mossakowski 2008).
The video below, “The Intersection of Race and Mental Health,” presents some of the newest research on race and mental health. It specifically calls out racial trauma as a cause of mental health issues.
Racial trauma is used to describe the physical and psychological symptoms that people of color often experience after being exposed to stressful experiences of racism (Jernigan et al. N.d.). For instance, people of color experience discrimination in the form of microaggressions, redlining, criminalization, and disproportionate incarceration. These experiences, and many others, contribute to racial trauma.
Further, nearly 36% of people who experience any mental illness and report as two or more races (SAMHSA 2021), meaning that they are mixed race or multiracial. We’ll look at two factors that might influence the mental health of multiracial people: Legal history and double-discrimination, although there are many more contributing factors.
People from different races have always had relationships with each other. Sometimes, in the cases of slavery, these relationships were non-consensual sexual violence. The laws against miscegenation, or the mixing of two races, were only overturned at the federal level in the US only in 1967 (Greig 2013). In fact, “the 2000 Census was the first time that citizens of the United States could select multiple racial categories for self-identification apart from Hispanic ethnicity in a census” (Whaley and Francis 2006). The lack of legal, governmental, and systems recognition of multiracial identity is an additional stress for multiracial people. If you would like to learn more, check out this blog, Laws that Banned Mixed Marriages.
A second contributing factor to mental health risks for multiracial people is double-discrimination, a concept which describes the experience of discrimination from both of one's communities. This popular media article about Kamala Harris quotes Diana Sanchez, a professor who studies multiracial identity:
"Sanchez says that multiracial people can face what she refers to as double discrimination, where they experience discrimination from both communities they are members of. In Harris’s case, that leads to South Asians saying she’s not South Asian enough and Black people saying she might not be Black enough. 'So there’s all these different sources of discrimination that are affecting the development of your multiracial identity and your experience with it, and that can make it hard to navigate,' Sanchez said" (Chittal 2021).
If you want to learn more about the experience of mixed-race people, check out Do All Multiracial People Think the Same?. Then answer the question: Why might mixed-race people have a unique experience of social problems, including mental health and mental illness?
Gender/Sex
In this subsection, we use the language of both gender and sex. Sociologists typically speak of gender, because it is the socially constructed gender roles and expectations that create differences between women and men (in a binary construction of gender which research often uses). However, regarding health, there are some biological sex differences between females and males (once again, this is binary because that is how health research has categorized bodies despite that intersex people have always existed). Interestingly though, some of those 'sex differences' are a product of the social construction of gender.
The evidence on gender/sex and health is both complex and fascinating. Women outlive men by more than five years, and the difference in longevity persists across racial categories. At the same time, women have worse health than men in many areas. For example, they are more likely to suffer from migraine headaches, osteoporosis, and immune diseases such as lupus and rheumatoid arthritis. Women thus have more health problems than men even though they outlive men – a situation commonly known as the morbidity paradox (Gorman & Read 2006). Why, then, do women outlive men? Conversely, why do men die earlier than women?
Several reasons explain the gender gap in longevity. One might be biological, as the estrogen levels of people assigned female and other sex-linked biological differences may make them less susceptible to heart disease and other life-threatening illnesses, even as they render them more vulnerable to other health problems (Kuller 2010). However, as with other differences in health outcomes, much of the difference may be due to social factors.
A second reason is that men lead more unhealthy lifestyles than women because of differences in gender socialization. For example, men are more likely than women to smoke, to drink heavily, and to drive recklessly. All such risk behaviors make men more vulnerable than women to life-threatening illnesses and injuries. Men are also more likely than women to hold jobs in workplaces filled with environmental and safety hazards that kill thousands of people annually – most of them men.
A final reason is men’s reluctance to discuss and seek help for their medical problems (see Baker et al. 2014), owing to their masculine socialization into being “strong, silent types.” Just as men do not like to ask for directions, as the common wisdom goes, so do they not like to ask for medical help. As one physician put it, “I’ve often said men don’t come in for checkups because they have a big S tattooed on their chests; they think they’re Superman” (Guttman 1999: 10).
Studies also find that men are less likely than women to tell anyone when they have a health problem and to seek help from a health-care professional (Emmers-Sommer et al. 2009). When they do visit a physician, men ask fewer questions than women do. In one study, the average man asked no more than two questions, while the average woman asked at least six. Because patients who ask more questions get more information and recover their health more quickly, men’s silence in the exam room may contribute to their shorter longevity (Foreman 1999). Interestingly, the development of erectile 'dysfunction' drugs like Viagra may have helped improve men’s health, as men have had to see a physician to obtain prescriptions for these drugs when otherwise they would not have seen a physician (Guttman 1999).
We have just discussed why men die sooner than women, which is one of the two differences that constitute the gender morbidity paradox. The other difference concerns why women have more nonfatal health problems than men. Several reasons explain this difference (Read & Gorman 2010). One reason arises from the fact that women outlive men. Because women are thus more likely than men to be in their senior years, they are also more likely to develop the many health problems associated with old age. This suggests that studies that control for age (by comparing older women with older men, middle-aged women with middle-aged men, and so forth) should report fewer gender differences in health than those that do not control for age, and this is indeed true.

Women more than men tend to have more health problems that are not life threatening. Two reasons for this gender difference are gender inequality in the larger society and the stress accompanying women’s traditional caregiving role in the family.
© Thinkstock
However, women still tend to have worse health than men even when age is taken into account. Medical sociologists attribute this difference to gender inequality in the larger society (Read & Gorman 2010). For example, women are poorer overall than men and more likely to be in poverty. As already noted, poverty is a risk factor for health problems. Women’s worse health, then, is partly due to their greater likelihood of living in or near poverty. Because of their gender, women also are more likely than men to experience stressful events in their everyday lives, such as caring for a child or aging parent. Their increased stress impairs the immune systems and thus worsens their health. It also is an important cause of their greater likelihood of depression and the various physical health problems (weakened immune systems, higher blood pressure, lack of exercise) that depression may cause.
Another reason is because women experience sexism – systemic, institutionalized discrimination – in their everyday lives, and (as is also true for people of color and racism) this discrimination is thought to produce stress and thus poorer physical health (Landry & Mercurio 2009). Women are affected adversely both by institutionalized sexism within and unequal access to the healthcare industry, which reflects gender inequality more broadly. According to a report from KFF, women experienced a decline in their ability to see needed specialists between 2001 and 2008. In 2008, one-quarter of women questioned the quality of their healthcare (Ranji & Salganico 2011). Quality is partially indicated by access and cost. In 2018, roughly one in four women (26%) compared to one in five men (19%) reported delaying healthcare or letting conditions go untreated due to cost. Because of costs, approximately one in five women postponed preventive care, skipped a recommended test or treatment, or reduced their use of medication due to cost (Ranji, Rosenzweig, and Salganicoff 2018).
In addition, many critics also point to the medicalization of women’s issues as an example of institutionalized sexism. Medicalization refers to the process by which previously normal aspects of life are redefined as pathological and needing medical attention. Many aspects of women’s lives have been medicalized, including premenstrual syndrome, menstruation, pregnancy, childbirth, and menopause. The medicalization of pregnancy and childbirth has been particularly contentious in recent decades, with many women opting against the medical process and choosing natural childbirth as part of their reproductive health plan.
Reproductive health is not limited to pregnancy and childbirth. It also includes the ability to choose when or whether to be pregnant. For centuries, women have controlled conception and pregnancy using plants and devices. As women’s bodies became more medicalized, contraception and termination of pregnancy became managed by doctors. In some cases, this was useful. Doctors developed 'the pill' in the 1950s, and it was widely available by the 1970s (Liao and Dolin 2012). By reliably preventing conception, women had more choices in when to get pregnant, at least once they didn't need permission from their husbands to take the pill. Often, this gave them more freedom to work, make money, and gain economic power.
The technology to provide safe, effective terminations of pregnancy also evolved. Abortion is the spontaneous or voluntary termination of pregnancy. As women fought to control their own reproduction, the right to choose abortion became a hotly contested debate. In early 1973, the Supreme Court affirmed the right to a woman’s privacy in matters surrounding her pregnancy in a 7-2 decision, commonly known as Roe v. Wade. The decision reads in part:
"The Due Process Clause of the Fourteenth Amendment protects against state action the right to privacy, and a woman’s right to choose to have an abortion falls within that right to privacy. A state law that broadly prohibits abortion without respect to the stage of pregnancy or other interests violates that right. Although the state has legitimate interests in protecting the health of pregnant women and the 'potentiality of human life,' the relative weight of each of these interests varies over the course of pregnancy, and the law must account for this variability" (Oyez N.d.).
For five decades after the Roe decision, women had access to abortion services in all US states. With access to safe and effective abortion, women’s health outcomes improved. Maternal mortality decreased, and there was less infant mortality (World Health Organization 2021).
However, some people did not agree with this legal decision. The conflict in values is based on politics, religion, and power. If you look at the conflict based on political party, you see that the Republican party argues that the unborn child has a right to life that cannot be violated. The Democratic party argues that people have the right to bodily autonomy, and to choose whether to get pregnant or to terminate pregnancy and to have access to safe, legal, affordable contraception and abortion.
However, not all Republicans and Democrats support their own party’s platform. Republicans who do support the platform are likely to be Protestant. Forty percent of them are white Evangelical Christians. Republicans who don’t support the right to life are much less likely to be religious. Eighty percent of Democrats support the right to choose. The 20% who don’t are commonly white Evangelical, Hispanic Catholic, or Black Protestant. The combination of race and religion appears to have a unique influence on beliefs about reproductive rights (Lipka 2022).
But differences in politics and religion mask a deeper divide: The debate over who controls women’s bodies. This is an example of gendered social control, the social control of women or people assigned female. Generally, men make the laws that control women and pregnant people’s bodies. We see the power of patriarchal systems in the challenges to Roe v. Wade. In the summer of 2022, access to abortion was removed as a federally protected right, as our right to privacy was dismantled (for all of us, not just women or pregnant people). Each state could now decide whether abortions were legal or illegal, and many states limited access to abortion.
The Supreme Court’s decision to have states decide abortion rights has worsened health outcomes for women, particularly if they are poor or women of color. Women and pregnant people may be arrested in some states if they have abortions. Doctors may face legal charges if they take action to terminate pregnancies, even when it is to save the life of the pregnant person. In October 2022, a doctor was concerned about legal action in one case where the fetus would not survive at birth. The woman endured “a roughly six-hour ambulance ride to end her pregnancy in North Carolina, where she arrived with dangerously high blood pressure and signs of kidney failure” (Kusisto 2022). Because poor women and women of color (who are disproportionately poor) can’t afford to travel to states which protect abortion rights, they are even more at risk.
The medicalization of health, particularly regarding reproductive health, encourages some women and pregnant people to work for reproductive justice, a framework that centers the human right to have children, not have children, and parent the children we have in safe and healthy environments (Beaumonis and Bond-Theriault 2017). This framework, developed by Black feminists, centers people with marginalized identities who are most at risk, and emphasizes how reproductive health is tied to intersecting oppressions. If you want to learn more about reproductive justice, watch the video What is Reproductive Justice?.
Gender is also related to mental illness in complex ways. Worldwide, women are more likely than men to experience mental health issues (Andermann 2010). The charts below shows the prevalence of Any Mental Illness (AMI) and Serious Mental Illness (SMI) among adults in 2020, two broad categories to describe mental illness conditions. AMI encompasses all recognized mental illnesses, whereas SMI is a smaller and more severe subset of AMI. There are some group-level differences in this data that are important to notice. One is that the prevalence of AMI and SMI among women is much higher than that of men – why might this be?
Social scientists consider social and structural factors. In the optional article, Culture and the social construction of gender: Mapping the intersection with mental health, psychiatrist Lisa Andermann calls us to look beyond individual explanations of women’s mental health and explore structural factors:
"Identifying the psychosocial factors in women’s lives linked to mental distress, and even starting to take steps to correct them, may not be enough to reduce rates of mental illness or improve well-being of women around the world. More studies which take into account the interaction between biological and psychosocial factors are needed to explore the perpetuating factors in women’s mental health, and explain why these problems continue to persist over time and suggest strategies for change. And for these changes to occur, health system inadequacies related to gender must be addressed" (Andermann 2010).
The nature of the relationship between gender/sex and mental health also depends on the type of mental illness. Women have higher rates of eating disorders and PTSD than men and are more likely to be seriously depressed, but men have higher rates of antisocial personality disorders (a lack of empathy, or psychopathy) and substance use disorders that lead them to be a threat to others (Christiansen, McCarthy, and Seeman 2022; Kort-Butler 2009).
Sociologists again attribute these differences to gender socialization that lead women to keep problems such as anger inside themselves while encouraging men to express anger outwardly, often through violence (Kessler and Wang 2008). To the extent that women have higher levels of depression and other mental health illnesses, the structural and cultural factors that account for their poorer physical health, including their higher rates of poverty and stress and rates of everyday discrimination, are thought to also account for their poorer mental health (Read & Gorman 2010).
We also return to patriarchy as an underlying contributor to health problems among women, nonbinary, and queer people below.
Sexuality and Gender
Gender and sexual identities may also impact how a person experiences health and illness. However, understanding these unequal experiences based on sociological data is challenging. Because being queer (including transgender) was stigmatized and under strict social control until recently in the US, many people did not and still may not disclose their identities as queer. The agencies that collect data about gender and sexual identity have only recently begun to re-tool their data collection methods so that people can report their identities accurately. Despite these limitations, though, we see inequality.
Queer adults have higher rates than heterosexual cisgender adults of physical health problems and also of mental health problems (Frost, Lehavot, & Meyer 2011; Institute of Medicine 2011). These problems are thought to stem from the stress that queer people experience from living in a society in which they frequently encounter verbal and physical harassment, job discrimination, a need for some to conceal their identity, and lack of equal legal treatment. Queer secondary school students experience various kinds of educational and mental health issues because of the mistreatment they encounter in the institution of education, and by the time that queer individuals reach their adult years, the various stressors they have experienced at least since adolescence have begun to take a toll on their physical and mental health.
Because stress compromises immune systems, queer individuals on average may have lower immune functioning and lower perceived physical health than heterosexual cisgender individuals. Because stress impairs mental health, they are also more likely to have higher rates of depression, loneliness, low self-esteem, and other psychiatric and psychological problems, including suicidality (Sears & Mallory 2011). Among all queer individuals, those who have experienced greater levels of stress related to their sexuality have higher levels of physical and mental health problems than those who have experienced lower levels of stress.
It is important to keep in mind that these various physical and mental health problems do not stem from a queer identity itself, but rather from the experience of living as a queer individual in a heterosexist and cissexist society. The American College of Physicians highlights the connections between laws, discrimination, and rejection that result in poorer health outcomes for queer people:
"These laws and policies, along with others that reinforce marginalization, discrimination, social stigma, or rejection of LGBT persons by their families or communities or that simply keep LGBT persons from accessing health care, have been associated with increased rates of anxiety, suicide, and substance or alcohol abuse" (Daniel & Butkus 2015).
Transgender people have unique health concerns that are rarely addressed well by current practices. Although transgender people differ in their desires regarding medical support for their physical transitions, many of the procedures are not covered by insurance. When examining health outcomes for transgender people, the report states:
"Transgender persons are also at a higher lifetime risk for suicide attempt and show higher incidence of social stressors, such as violence, discrimination, or childhood abuse, than nontransgender persons. A 2011 survey of transgender or gender-nonconforming persons found that 41 [percent] reported having attempted suicide, with the highest rates among those who faced job loss, harassment, poverty, and physical or sexual assault" (Daniel & Butkus 2015).
Newer research is focusing on the interactions of nonbinary and genderfluid individuals and their mental health. The video below discusses the intersection of gender identity and mental illness.
In this episode of All Things Considered: Health Care System Fails Many Transgender Americans, the journalist notes that simple things, like having forms that indicate only 'male' and 'female' (which assumes that everyone is cisgender and fails to represent both intersex and transgender people), become barriers to accessing health care services. Transgender people are more likely to experience preventable health conditions because it is difficult to find medical providers who will treat them with respect. The videos that are linked to this episode explore issues related to transgender health in more detail.
Personal Profile
In the piloting of the Puttman et al. textbook that was incorporated into the textbook you're now reading, one student who participated in the open pedagogy project expanded our collective understandings of gender and sexual identity. They shared their own experiences of gender identity and created art to convey the prejudice that they experience from the medical community.
The image below conveys the understanding of the physician that gender can only be experienced as a binary and the limited belief that transitioning means to fulfill one of those two gender identities. When you examine the picture from the perspective of the trans person, you see both a key and a chain. The chain represents how a trans person is often chained to the binary during medical transition. The key represents how a trans nonbinary person would want to break away from the binary the medical system puts on them in order to meet the transition goals they actually have.
The student writes:
Being able to be a part of progress for the future and being able to influence the learning of people like me who take Sociology was an unexpectedly heart-warming experience. During the class itself, it didn’t feel that impactful. However, as the class was coming to a close, I got the sense that my, and the rest of my class, were going to change the class just as much as the class changed us.
I also got the opportunity. After noticing a gap in knowledge in the textbook about medical discrimination for trans people, I wrote an essay detailing the issues that trans people like myself deal with while trying to transition. While it was relevant then, it seems even more relevant now. When asked to elaborate artistically, as a nonbinary person myself, I was able to delve more into the feelings associated with such discrimination – frustration, helplessness, anger and shame. After sharing this essay and the art pieces illustrating my points, I felt that my efforts were actually going to do something beyond fulfilling the necessities of the assignment.
This experience in open pedagogy supported the student in telling their truth. Their classmates were able to learn from this example. One student even changed the topic of her paper from 'women’s reproductive rights' to 'people’s reproductive rights,' to honor the fact that not all people with uteruses are women. And, because this art and essay can be incorporated into the course and textbook, future students are able to benefit.

“So, you want to transition?” is student-created artwork. They illustrate that the doctor holds a binary understanding of gender identity. The person looking to transition, meanwhile, is trapped by those options because they are nonbinary.
“So, you want to transition?” © EME, Soc 205 and 206 Student, is all rights reserved and included with permission
Despite the health problems that queer people experience, medical students do not learn very much about these problems. One survey of medical school Deans found that one-third of medical schools provide no clinical training about these health issues, and that students in the medical schools that do provide training still receive only an average of five hours of training (Obedin-Maliver et al. 2011). The senior author of the study commented on its findings, “It’s great that a lot of schools are starting to teach these topics. But the conversation needs to go deeper. We heard from the deans that a lot of these important LGBT health topics are completely off the radar screens of many medical schools” (White 2011).
When the Centers for Disease Control and Prevention (CDC) examined risk factors for COVID-19 illness or death, they found that lesbian, gay, and bisexual (LGB) people had challenging underlying health conditions more often than straight people (see the figure below). The report points primarily to economic causes as a core cause of the difference, indicating that LGB people, particularly if they are Black or Brown, experience more economic instability (Heslin & Hall 2021).
In addition to concerns such as economic instability, stress, and stigma, we must consider cultural factors in explaining the poorer health of queer individuals and women.
Like our concept of structural racism, our society is structured on patriarchy: A structural system that positions (white) men and masculinity above all others. Alda Facio, a Costa Rican jurist, writer, teacher, and activist, offers the following definition of patriarchy:
"Patriarchy is a form of mental, social, spiritual, economic and political organization/structuring of society produced by the gradual institutionalization of sex-based political relations created, maintained and reinforced by different institutions linked closely together to achieve consensus on the lesser value of women and their roles" (Facio 2013).
Patriarchy is the social structure and related behaviors that give men power and that oppress women and nonbinary people, as well as queer people more broadly because it normalizes heterosexuality. As social problems scholars, we want to understand how patriarchy works in a much deeper way. Examine the image below:

Patriarchy is like a tree. It has the roots of core principles, the trunk of institutions, the branches of social interactions, and the leaves of individual behavior.
See photo credit above
In the drawing of this tree, we notice:
Roots: The roots of the patriarchal tree are the core beliefs and practices that provide an often unconscious base of patriarchy. These underlying principles are obsession with control – controlling women’s bodies, money, and choices. This principle also supports the idea that men should stay in control, of their emotions, lives, and other people’s lives. The second principle, male domination, locates men in positions of authority. Leadership is a male role and a source of male power. The third principle, male identification, locates men at the center of what is right and good. We see this principle in action when we use words like all mankind when we actually mean all people. The fourth and final principle is male centeredness, which focuses on and value the activities of men and boys, rather than women, girls, and nonbinary people. Combining many of these principles in action, the US Soccer Federation agreed that women and men soccer players should earn equal pay, as of 2022. For more on this landmark victory, feel free to read The US National Women’s Soccer Team wins $24 million in equal pay settlement.
Trunk: The trunk of this structural inequality are our institutions, our governments, and our economy. Throughout this book, we have seen examples of gender inequality, often supported by our schools, businesses, and governments. We’ve also seen how these organizations sometimes change to become less patriarchal.
Branches: The branches of our tree are the smaller containers of social interaction, such as families, churches, clubs, work teams, or your favorite gamer’s discord group. At this level, group norms influence the behavior of individuals. In these smaller communities, we explore what it means to 'do' the gender of nonbinary, woman, or man. For example, in many heterosexual dual-parent families, members take on traditional gender roles.The father mostly does outside chores like mowing the lawn or taking out the trash, and the mother does more of the ongoing daily tasks of cleaning up, laundry, and family planning.
Leaves: Each of us is a leaf on the patriarchal tree. In our own actions, we can reinforce gender norms, or we can consciously choose to uproot these deep roots. Our choices matter deeply. However, by placing each of us in a system of power, we move away from shame, blame, and a bad person model. Instead, we can examine how social structures of gendered oppression may be reproduced in our own daily interactions. This knowledge empowers us to choose differently.
Because this structure is both deeply rooted and interconnected, it is resistant to change. Also, patriarchy itself becomes a reason for inequality in all of our social problems.
Again, it is not gender or sexual identity that causes poorer health outcomes. Instead, it is the social structure embedded with stigma, discrimination, and violence that makes life riskier and shorter for queer people.
Age
Health is quite obviously related to age, in that physical and cognitive health declines as we get older. Rather than focusing on that connection, we will explore the relationship between young age and mental health.
While 21% of all adults have a mental illness, almost half of all teenagers have mental disorders, as demonstrated in the figure below.

This chart shows the prevalence of Any Mental Disorder among adolescents. Almost half of all teenagers report a mental disorder. What do you think might cause such a high rate?
“Prevalence of Any Mental Disorders Among Adolescents” by the National Institute of Mental Health is in the Public Domain
Why is there such a wide difference between teenagers and adults? It’s hard to say for sure, but research offers three options:
First is biology: Scientists are mapping changes in the brain in much more detailed ways. During adolescence, the brain adds new connections, particularly connections related to executive planning and regulation. Half of adults with mental disorders experience onset of the disorder by age 14, and 75% of adults experience onset by age 24 (Kessler 2007). Remembering that the human brain is in formation until age 25, these data suggest that experiences during adolescence shape mental health outcomes. Let’s look deeper.
Scientists are mapping brain development in new ways that reveal the importance of the neural networks that are being created in adolescence. An adolescent brain is creating new connections, particularly connections related to planning and regulation. These connections help to stabilize a person’s mental health. Further, if a person’s experience or biology does not map new connections in essential pathways, a person’s mental health may be less stable. Because adolescent brains not only respond to the same experiences as adult brains, but develop faster and more extensively, experiences in adolescence may shape the brain’s functioning more powerfully than those some experiences in adulthood. Experiences that negatively impact brain development include child and adolescent illness, hormonal shifts, exposures to toxins such as drugs and alcohol, food insecurity, trauma history, emotional and physical abuse. As discussed below adverse childhood experiences (ACEs) predict health outcomes. Impact on brain development is one of the ways in which childhood trauma impacts adult health outcomes. Specifically, trauma and stress factors negatively impact normal brain development and increase vulnerability to mental or emotional illness.
Second is exclusion in data: Other researchers suggest that part of the difference between the two age groups has to do with being able to contact people. Many youth are still connected with school and family, even if they are experiencing mental health issues. Most mental health surveys don’t contact people in residential living, including assisted living, group homes, prisons, or jails. Also, they do not contact people who are houseless. Because of this, mental health issues in adult and senior populations may be significantly under-reported (Kessler & Wang 2008).
Third is the question of more stress or less stigma: Researchers are exploring whether the increase in reporting of mental health issues for teens and young adults is due to experiencing more stressors or experiencing less stigma around reporting mental health concerns. This article, Why Gen Z is More Open in Talking about Their Mental Health explores this conundrum; feel free to read it if you like.
Global Perspective
The nations of the world differ dramatically in the quality of their health and healthcare. People in poorer nations suffer from low nutrition, unsafe water, inadequate sanitation, rampant disease, and inadequate health care. One disease they suffer from is AIDS. Some 34 million people worldwide have HIV/AIDS, and two-thirds of these live in sub-Saharan Africa. Almost two million people, most of them from this region, died in 2010 from HIV/AIDS (World Health Organization 2011). All these health problems produce high rates of infant mortality and maternal mortality and high death rates. For all these reasons, people in the poorest nations have shorter life spans than those in the richest nations.

Two-thirds of the 33 million people worldwide who have HIV/AIDS live in sub-Saharan Africa. This terrible fact illustrates just one of the many health problems that people in poor nations suffer.
khym – AIDS Orphans and their Guardians in Sophia Village near Nairobi, Kenya – CC BY 2.0
A few health indicators should indicate the depth of the problem. Life expectancy is one important measure of a nation’s health and is relevant for understanding worldwide disparities in health and health care. North America, Western Europe, Australia, and New Zealand have much longer life expectancies (75 years or more) than Africa and Asia, where some nations have expectancies closer to 60 or fewer years. The society we live in can affect our life span by more than a quarter of a century. In 2023, country life expectancy at birth ranged from a low of 54 years in Nigeria to a high of 86 years in Monaco and San Marino (World Bank Group n.d.).
The figure below compares another important indicator, infant mortality for nations grouped into four income categories. Though the gap has been closing and lower-income nations are faring far better than decades ago, striking differences persist. The rate of low-income nations is 12 times higher than that of high-income nations, at 6.1% versus 0.5%, respectively (United Nations 2025).

This chart illustrates how the child mortality gap by nation income level has been getting smaller; however, it has not yet closed and there remains a wide gap between low-income and high-income countries.
Source: Our World in Data 2025; United Nations 2025
Not surprisingly, these global differences are similar to those for adequate sanitation. Whereas the percentage of access to adequate sanitation facilities (i.e., the removal of human waste from the physical environment, as by toilets) is at least 98% in the wealthy nations of North America, Western Europe, Australia, and New Zealand, it is less than 33% in many poor nations in Africa and Asia.
Social Determinants of Health
As we have seen, social contexts including social inequalities account for much of the disparities we see in health by social class, race/ethnicity, gender, and sexuality. Sociologists and others who study human health have a detailed model that helps them make sense of health in these and other social groups. This model is called the social determinants of health. More specifically, the social determinants of health are the circumstances in which people are born, grow up, live, work, and age and the systems put in place to deal with illness (World Health Organization 2013). These circumstances are shaped by a wider set of forces: economics, social policies, and politics.
Social scientists and health professionals use this model of social determinants of health to describe the social factors that influence the health or lack of health of different social groups. The Centers for Disease Control (CDC) created the model image below. We see that access to quality health care influences how healthy you might be. Whether your neighborhood is located next to an oil refinery changes your health outcomes. You might be surprised that education access and quality also impact your health. Wealthy people can pay more money for healthcare. Additionally, they get better educations, which sometimes leads to better health choices.

This is a model of the Social Determinants of Health (SDOH), provided by the CDC. How do these factors impact your own health or the health of your family? How might these factors impact the health of families who are different from you?
“Social Determinants of Health Model” by the Centers for Disease Control (CDC) is in the Public Domain
The way organizations and institutions create models for the social determinants of health can change what we see. If you’d like to explore this question more deeply, here is a model from the World Health Organization and a SDOH model from the Canadian First Nations Peoples. Why might these models be different from each other?
In a slightly different social model of health, researchers look at how trauma over time affects health outcomes. Adverse Childhood Experiences (ACEs) are potentially traumatic events that occur in childhood (0-17 years). The ACEs model measures the amount of trauma a child experiences and describes the impact of trauma on health outcomes. Trauma is a person’s (or group) response to a deeply distressing or disturbing event that overwhelms one’s ability to cope.
The figure below shows the ACE Pyramid model distributed by the Centers for Disease Control and Prevention. ACEs potentially impact health outcomes later in life.

This images portrays the ACE pyramid. Many of us experience some adverse childhood events. When communities and families invest in protective factors, the impact of ACEs on our future health outcomes decreases.
See photo credit above
In the model image, an arrow on the side shows the progression from conception (at the bottom) to death (at the top). The levels, from conception to death, are:
- Generational Embodiment/Historical Trauma
- Social Conditions/Local Context
- Adverse Childhood Experiences
- Disrupted Neurodevelopment
- Social, Emotional, & Cognitive Impairment
- Adoption of Health Risk Behavior
- Disease, Disability, & Social Problems
- Early Death
When children experience trauma, their predicted health outcomes get worse. These adverse or traumatic experiences may include growing up in a family with mental health or substance abuse issues, child abuse, or other experiences of violence. Because a person who experiences these events is more likely to experience some physical and mental health challenges in childhood, they are more likely to adopt risky behaviors as an adult. Additionally, the more ACEs an adult has, the more it can predict that person’s risk of developing health problems such as diabetes, heart disease, and cancer. If left untreated, the related diseases and disabilities can lead to early death.
However, when children get help from caring adults, are connected with others, or receive competent professional support, they can recover from this early trauma. These interventions and others are known as protective factors. If families and communities support children with protective factors, the negative health impacts of trauma decrease. Many people experience at least one Adverse Childhood Experience in their lifetime. However, people in marginalized social locations have more risk of ACEs.
Beyond the experience of an individual, generational embodiment or historical trauma contributes to the likelihood of future generations of social groups experiencing ACEs. Historical trauma is multigenerational trauma experienced by a specific cultural, racial or ethnic group (Administration for Children and Families N.d.). It is related to major events that oppressed a particular group of people because of their status as oppressed, such as slavery, the Holocaust, forced migration, and the violent colonization of Indigenous people in North America. The generational embodiment of this trauma means that trauma responses of a previous generation are passed down to future generations unless they are healed.
For a deeper look at how ACEs work, you may watch the TED Talk, How Childhood Trauma Affects Health Across a Lifetime.





















